Rapid Relief for mood and pain disorders
Ketamine is a well researched, dissociative anesthetic that was approved by the FDA in 1970. Since then, Ketamine has been used extensively for pediatric and adult treatment in surgery, emergency departments, ambulances, trauma medicine, and war zones. The World Health Organization lists Ketamine as one of the most essential medications due to its therapeutic effects and wide margin of safety. Over the last decade, Yale University and the National Institutes of Health identified additional benefits of Ketamine in treatment of mood disorders and chronic pain. The use of Ketamine for depression has been named "The biggest discovery in mental health in decades."
"Recent data suggest that ketamine, given intravenously, may be the most important breakthrough in anti-depression..."
How does it work?
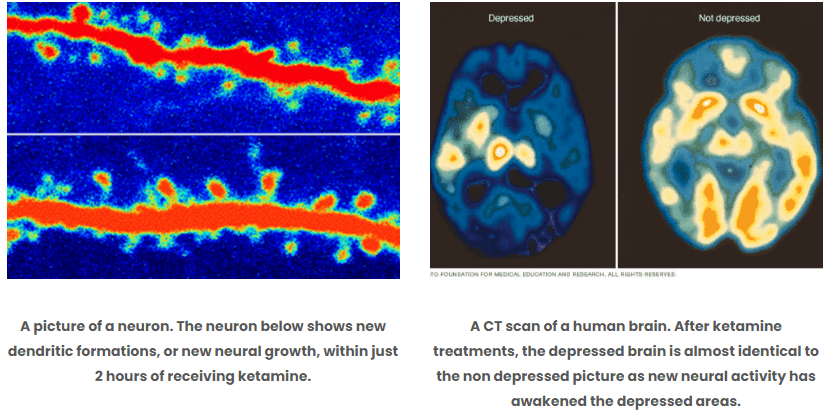
Ketamine, originally an anesthetic, has gained attention for its potential in treating mood disorders, depression, and chronic pain. It appears to work by impacting glutamate neurotransmission, rapidly improving mood by promoting synaptic plasticity and resetting neural circuits. In addition to its antidepressant effects, ketamine can induce elevated mood, reduce negative emotional states, and potentially modulate emotional processing. However, its use should be closely supervised by healthcare professionals due to the risk of dissociative and hallucinogenic effects and potential abuse. Ketamine treatment is typically administered in controlled clinical settings tailored to individual needs and responses.
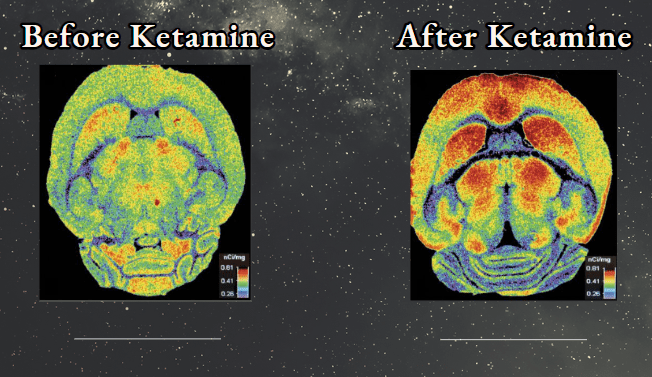
It is also used in pain management by blocking NMDA receptors, which reduces pain perception and central sensitization. It can also enhance the effects of opioids, potentially allowing for lower opioid doses and reducing associated side effects and addiction risks. Ketamine shows promise in managing chronic pain, but it should be administered under medical supervision in controlled settings to ensure safety and mitigate potential side effects.
What kind of results can I expect?
Ketamine therapy can yield varying results for individuals with conditions like depression, OCD, PTSD, chronic pain, suicidal ideation, and anxiety. Many report rapid and significant improvements in mood, reduced symptoms, and increased quality of life. For some, ketamine provides relief when other treatments have failed, making it a valuable option for treatment-resistant cases. However, the extent of improvement can vary from person to person, and the effects may not be long-lasting, requiring periodic treatments. Close monitoring and ongoing care by healthcare professionals are essential to assess and optimize the outcomes of ketamine therapy while considering potential side effects and individual responses.